The ancient origins of anthrax date back as far as 700 BC. Meanwhile, the first clinical description of anthrax was as early as 1752. By the late 1800s, scientists were making huge strides within medicine, and one such stride included Louis Pasteur’s creation of the first vaccine for anthrax. Hundreds of years ago, we primarily knew anthrax as an economic nightmare as it ravaged domesticated animals like our livestock.
Of course, trends from past decades can be delightful when they return to inspire today’s music, fashion, and art. However, a dangerous blast from the past in the form of anthrax has reared its ugly head. In early August 2021, China reported a case of the deadly Anthrax pneumonia – its first case after ten years [1]. A few weeks later, local health authorities in another Chinese province discovered nine suspected cases of Anthrax [2]. Around the same time, Russia confirmed a case of Anthrax with a cutaneous infection in a patient involved in butchering cattle meat [3]. These particular anthrax outbreaks aren’t all the disease is known for; there are many ways that anthrax makes its way to the public eye, including popular culture or pop culture.
Bioterrorism and Hollywood seem to go hand-in-hand. Viruses and bacteria in biological weapons have infected the storylines of science-fiction movies and books for decades. From AIDS to Ebola to West Nile Virus, the United States has been obsessed with the concept of “killer germs.” After September 11, 2001, a new era of “killer germs” started making waves in modern pop culture. This is directly related to the “Anthrax by Mail” attack, which took place in the days and weeks following 9/11, which we will look at in more detail later. So, considering these events and the fascinations of our culture. Is it a surprise that so many movies, TV shows, and books show a distinct theme of disease apocalypse? Maybe not, but the real question then becomes, is this obsession and fear of an apocalypse by anthrax with good reason?
What is Anthrax?
The gram-positive bacteria Bacillus Anthracis causes anthrax; therefore, anthrax is also commonly known as B. anthracis. The bacterium gets its name from the Greek word for coal, “anthrakis,” because it often results in black lesions on the skin. This bacterial rod is highly resistant to inactivation and is often present in the soil for decades. It most commonly affects agricultural animals such as sheep, cattle, and goats, but it can also infect humans.
One of the first reported anthrax cases dates back to the early 1800s, when an outbreak occurred in Italy. However, the disease is thought to have existed for centuries before this. Another early reported anthrax case dates back to 1876, when an outbreak occurred in wool mills in Yorkshire, England.
Luckily, the infection is not spread rapidly from person to person through the air like the flu or cold. It can, however, cause severe illness in domestic animals and humans if they interact with infected animals or contaminated animal products. There are three main types of anthrax: cutaneous, inhalation, and gastrointestinal.
Gastrointestinal
It is not as common as some other types of infection. Still, anthrax can also be found in the gastrointestinal system known as the esophagus, stomach, and intestines of someone who recently had raw or undercooked meat contaminated with B. anthracis. The bacteria that cause anthrax produce toxins that damage the lining of your stomach and intestine. This can lead to severe inflammation, bleeding, and even death.
Early symptoms of gastrointestinal anthrax include:
- nausea
- vomiting
- abdominal pain
- fever
As the disease progresses, you may experience:
- bloody diarrhea
- dehydration
- shock
–
Although gastrointestinal anthrax is rare, it can be fatal if left untreated. Treatment typically involves antibiotics and supportive care. With prompt treatment, the prognosis for patients with gastrointestinal anthrax is generally good. In some cases, surgery may also be necessary to remove infected tissue. Early diagnosis and treatment are essential for the best possible outcome. People can also become infected through contact with infected animal products, such as meat or hides.
Cutaneous
Cutaneous anthrax occurs when the bacteria enter through a break in the skin, usually via a cut or abrasion. The most common natural way people get a Bacillus Anthracis infection is cutaneous, after skin contact with contaminated meat, wool, or leather from infected animals. Cutaneous Anthrax infection can be transferred through open lesions from one person to another.
The initial symptom is usually a small, raised bump that resembles an insect bite. The bump develops into a blister that fills with pus and eventually ruptures within a few days, leaving an ulcer. Other symptoms may include:
- fever
- fatigue
- swollen lymph nodes
- Itchy blisters or bumps
–
In some cases, the lymph nodes may also be more severely affected. If left untreated, cutaneous anthrax can be deadly; however, prompt treatment usually effective. Treatment typically involves antibiotics and supportive care. If you think you may have been exposed to anthrax, it is essential to seek medical treatment immediately.
Inhalational Anthrax
Inhalation anthrax occurs when people inhale airborne spores of the bacteria. This is the most severe and rare form of human anthrax, with a fatality rate of 80% and above. It is fatal unless treated immediately. Inhalation of Bacillus Anthracis spores is not common in nature. Anthrax spores can be released into the air and breathed in, causing the lungs to become inflamed. Symptoms of inhalation anthrax include:
- fever
- chest pain
- difficulty breathing
- coughing up blood
- dizziness
- extreme fatigue
–
Like the other forms of the disease, inhalational anthrax can be fatal if left untreated. Early diagnosis and treatment are essential for the best possible outcome. Treatment typically involves a combination of antibiotics and supportive care. Anthrax is a rare but potentially deadly disease that should be taken seriously. If you think you may have been exposed to anthrax spores, seek medical attention immediately. Another unique aspect of this form is that this method has been exploited throughout history for bioterrorism purposes.
Bacillus Anthracis: A Dark History of Bioterrorism
Bacillus Anthracis is effective as a weapon primarily because of its spores. In nature, an infected host sheds the spores on the ground, which then multiply on contact with air. These spores can stay dormant for years, even decades, in the soil, waiting for another host [4]. The infection cycle then continues. However, when these microscopic spores can be aerosolized as sprays or powders, they can be released silently and escape detection. Even a small number of spores released in the air can infect massive numbers of people.
One of the most well-known instances of Anthrax used as a biothreat was in the United States. This instance is commonly known as the “Anthrax by Mail” attack, which took place in the days and weeks following 9/11. During this attack, a powder with anthrax spores was sent via the United States Postal Service to at least two senators and various news agencies across the East Coast. The powder allowed the spores’ easy inhalation, which mainly went unnoticed until the first anthrax diagnosis on October 4, 2001. By the end of the outbreak, 10,000 people had been at risk of exposure, 43 people had been confirmed to be exposed, 22 people were ill, and 5 of them had died. This attack, formally known as the Amerithrax attack, led to a long-term investigation that did not end until 2010. It is considered one of the most extensive and most complicated investigations in U.S. history. They found their suspect after conducting more than 10,000 interviews on many continents and collecting over 5,730 environmental samples.
This is not the only time in which we’ve seen the diseases used in bioterror, in fact, it wasn’t even the first time. The earliest reports of weaponized deployment of anthrax come as early as 1914 during World War I. By 1960, there was serious concern about the possibility of anthrax as a bioterror agent. There was also concern about “lax” biosafety protocols in labs that handled dangerous agents like B. anthracis.
In 1979, one of the first globally reported outbreaks occurred in the USSR. This was a much larger Anthrax outbreak. Bacillus Anthracis spores were released from a Soviet military research center in Sverdlovsk, Russia. The story has all the intrigue and devastation characteristic of the Cold War. 60-70 people are estimated to have died from the accident, now termed the ‘Biological Chernobyl.’ Soviet officials at the time said the outbreak was due to naturally occurring anthrax and not concerning any use or study of biological weapons, however, many other officials around the globe felt this was an instance of bioterror that was covered up. It was only almost thirteen years later that a team of expert molecular biologists from Harvard University could investigate the spread of the spores on behalf of the CIA [5]. The team confirmed that aerosolized spores spread through the air and caused the outbreak, not meat. The outbreak was made up of over 90 cases, primarily gastrointestinal.
A review of the GIDEON Bioterrorism note for Anthrax shows a long murky past of the pathogen being released by countries during the war, terrorists to spread fear and destruction, or by accident.

Snippet of Bacillus Anthracis Bioterrorism Note from GIDEON database.
Anthrax Impacts Health on a Global Scale
Understanding the epidemiology, cross-border transmissions, and the history of this zoonotic pathogen is essential to help encourage safe practices when handling livestock and avert potential threats. Bacillus Anthracis infections have affected almost every corner of the globe. It is effortless for anyone to carry an infectious disease endemic to one country and spread it to others. Out of the 697 outbreaks that have been recorded, which can also be found in GIDEON, only ten have been cross-border events. So, when it comes to an anthrax outbreak, it is more likely to be related to naturally occurring anthrax from within its country of origin.
If we look even closer at the outbreaks, we can see that 91 countries have reported anthrax outbreaks. The European Region, as classified by the World Health Organization (WHO), has the highest amount of outbreaks while the Eastern Mediterranean Region has the lowest number. The European Region actually accounts for approximately 30% of all outbreaks globally despite the fact that India has the most outbreaks recorded by a single country. The year 2010 has the most recorded outbreaks with as many as 37 outbreaks occurring during the calendar year.
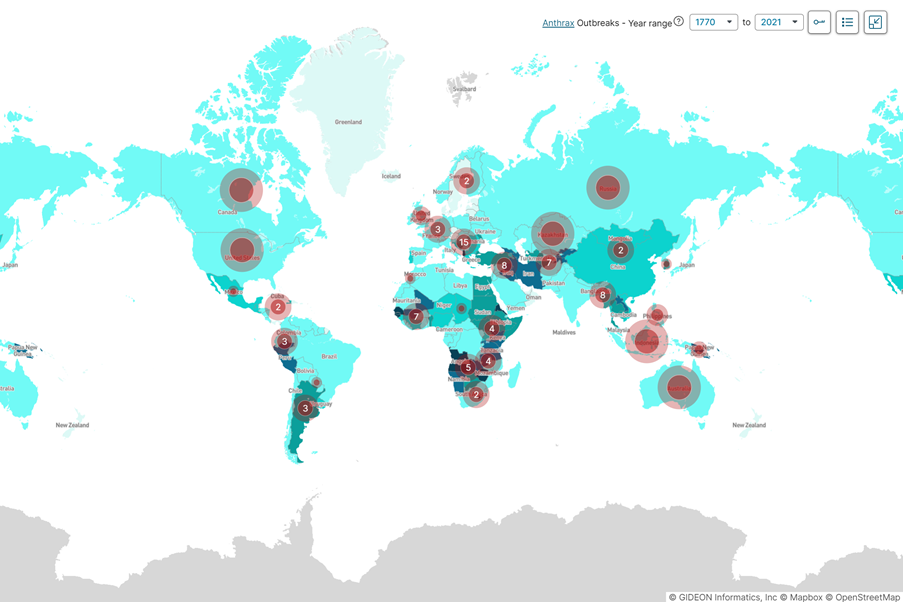
World map of Bacillus Anthracis outbreaks, 1770-2021
National public health agencies, frontline clinicians, infectious disease specialists, and microbiologists will have to work together to mitigate the effects of dangerous pathogens like the Bacillus Anthracis. Taking epidemiological data into account when diagnosing diseases in Point-of-Care settings can be a significant first step toward containing emerging infections. The United States, the U.K., E.U., and many other countries worldwide have implemented better tests and protocols around the way animals are handled. With these processes in place, cutaneous anthrax infections have significantly decreased.
The Vaccine
The anthrax vaccine was invented in 1881 by French chemist Louis Pasteur. It was the first vaccine ever created, and it was used to prevent anthrax infection in animals. The anthrax vaccine for humans was developed in 1954, and it is still used today. The vaccine is made from a killed form of anthrax bacteria. It is given in three doses over six weeks. It is injected into the skin or taken by mouth.
The anthrax vaccine is given to people at high risk for exposure to anthrax, such as people who work with animals or in laboratories. The anthrax vaccine is also given to military personnel and travelers. The anthrax vaccine is important because it can help in the prevention of anthrax infection. The vaccine is most effective when given before exposure to anthrax bacteria. However, it can also be given after exposure to help reduce the severity of symptoms. Like all diseases and disease control methods, prevention of the infection is the best medicine.
Should We Tremble in Fear of the Disease?
Anthrax as a bioterror agent has been a phenomenon that has spurred the imaginations of stories, films, and shows for decades. This project set out to determine if this is all hype around something improbable or if our morbid obsession with “killer germs” is founded in reality.
From a sample of 697 reported outbreaks spanning across the globe, it seems that the morbid curiosity is more founded in sensationalism than reality itself. There have only been three outbreaks reported due to bioterrorism-related events, which translates to 0.43% of all anthrax outbreaks. Not only that, but the statistical analysis shows that there is not a significant difference between the bioterror events across the world regions. This means that no one area of the world is statistically more likely than another to have a bioterror event related to anthrax based on this historical data alone.
The question remaining is whether we will see the killer germs like anthrax and Ebola continue to dominate pop culture, or will coronaviruses and the like take the mantle of Hollywood’s favorite doomsday germ after the pandemic?
The GIDEON Difference in Medical Research
GIDEON is one of the most well-known and comprehensive global health databases for infectious diseases. Data is refreshed daily, and the GIDEON API allows medical and health professionals and researchers access to a continuous stream of health data. Whether your research involves quantifying health data specifically for disease control, learning about specific microbes, or testing out medical differential diagnosis tools– GIDEON has you covered with a program that has met standards for accessibility excellence. You can also review our health based eBooks that feature medical notes on Loiasis, Miscellaneous Intestinal Protozoa, Onchocerciasis, etc. Or check out our global health status updates on countries like Morocco, Romania, Saint Kitts and Nevis, and more!
References
- “China Reports First Human Case of Pulmonary Anthrax in 10 Years,” Caixinglobal.com. [Online] [Accessed: 26-Aug-2021].
- Global Times, “Shanxi Province reports 9 suspected anthrax cases, treatment underway,” Globaltimes.cn. [Online] [Accessed: 26-Aug-2021].
- Press Release, “Human anthrax case reported in Karabudakhkent region, Russia,” Outbreaknewstoday.com, 10-Aug-2021. [Online] [Accessed: 26-Aug-2021].
- A. Chateau, S. Van der Verren, H. Remaut, and A. Fioravanti, “The Bacillus anthracis Cell Envelope: Composition, Physiological Role, and Clinical Relevance”, Microorganisms, vol. 8, no. 12, p. 1864, 2020. Available: 10.3390/microorganisms8121864 [Accessed 26 August 2021].
- “Anthrax at Sverdlovsk, 1979“, Nsarchive2.gwu.edu, 2017. [Online] [Accessed: 26- Aug- 2021].
- Epidemic entertainments: Disease and popular. – JSTOR. JSTOR. [Online][Accessed: 6-Dec-2021]
- History of anthrax. Centers for Disease Control and Prevention. [Online][Accessed: 6-Dec-2021]
- Amerithrax or anthrax investigation. FBI. [Online][Accessed: 6-Dec-2021]
- Anthrax – biological threat in the 21(st) Century. [Online][Accessed: 6-Dec-2021]
- Anthrax: A disease of biowarfare and public health importance. World journal of clinical cases. [Online][Accessed: 6-Dec-2021].
- World Health Organization, Fourth edition anthrax – world health organization. [Online][Accessed: 6-Dec-2021].